Your alarm goes off at 6am. You show up for work, with your list of about 13 patients. Your bedside nursing team greets you and everyone else by their first name. You have time to see everyone twice today, and sit in on two family meetings, while your colleague holds your pager. After rounds you report a medication error to leadership, and are rewarded for your attention to a culture of safety, which the hospital treats as a learning opportunity. During the day, a committee meeting on an improvement project that interests you starts on time and ends early. Your input is valued, as is everyone else’s at the meeting. At the session’s end, you are rewarded with a new title. Leadership reminds everyone the essential role for hospitalists and thanks them for another great quarter. Additionally, you are told your title comes with a new perk, no night call for 6 months, and 1 paid day to work on the project every month. You thank everyone for a great meeting, and then catch up with some team members from the hospital for dinner, family members included.
You come home, tell yourself it’s great to be a hospitalist, and set the alarm. It sounds at 6am and you wake up to find you have 25 patients to see, the EMR is frozen, no time for meetings, you break your records with 100 pages in a shift, you run into nurses who all seem like they just started this week, and rounding on about 2 patients per unit over 12 different units.
Which one is closer to your group?
Unfortunately, it feels like the nightmare of the latter is closer to the truth than the dreamworld of the first scenario. Though I think there is a piece of the former that is true: it’s great to be a hospitalist. And I don’t think we are far off to reach that version of hospitalist utopia. I’ve worked and talked with many hospitalists who are on track to achieve most of those high quality elements. We need to find ways to put it all together. If we reach that state, maybe the 50% burnout in our profession will reduce and we will have a more engaged profession trying to keep their home, the hospital, safe. To achieve a more perfect vision, we need to be engaged in our group, in our hospital, and we will achieve a fulfilled state.
Abraham Maslow founded humanistic psychology, searching for the roots of motivation. One of his most famous works is his hierarchy of needs shown below:
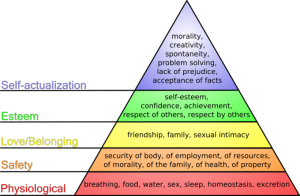
Maslow’s Hierarchy of Needs. See www.boundless.com
At the most basic level are physiological needs: food, sleep, water. Next, the level of security, followed by love, self esteem and then heading out to reach peak performance, which he labeled self-actualization.
Leadership at the hospitalists and hospital level need to understand that we will want to keep our house safe if given the opportunity. But if the census consistently reaches high levels, we just tread water.
I use Maslow’s hierarchy of needs for hospitalists as a guide towards engaging hospitalists, and helping hospitalists reach peak performance. SHM has a much more comprehensive way to measure engagement.
If you are struggling to piece together the elements that may squeeze more juice out of your docs, one strategy may be to do this type of assessment. See my simplistic transposition of Maslow onto the Messler’s Hospitalist Hierarchy of Needs below.
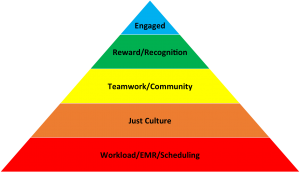
Messler’s Hospitalist Hierarchy of Needs
Maslow’s first level is physiological. What is your food and shelter? It is our census, our EMR, our scheduling, and other structural elements that keep us sane. Before you ask to be engaged in any aspect of the hospital, are you sure your schedule is balanced, that the census is not overloaded, leadership is supportive, and do you simply have an office to meet in? If level 1 is not met, your docs burn out quickly.
Once you reach that basic level, you can move to the next level and begin the process towards engagement and fulfillment. These next steps can occur in various orders, but I think a crucial element is the second level of security. In the hospital world, that means a culture of safety. If level 2 is not met, you have a hospital filled with pointing fingers, the blame game where the system is never the solution and the individual is always the problem. The errors begin to pile up because they are not reported, and no one wants to engage in improvement because no one believes the data and is worried about their job if they fight for a cause. Once you feel secure in a just culture, you’ll feel more confident you can safely measure, report, provide feedback, and improve your environment and patient care.
The third area is love, which in our context of the hospital resides in working well as a team, keeping the community in community hospital. Teamwork at the bedside, during team meetings, and at the committee level is essential. If level 3 is not met to some degree, then we are still practicing in 20th century “everyone for themselves” mentality, and miss out on the benefits of camaraderie, communication, continuous improvement and community.
At the 4th level are reward and recognition. Do you have a doc of the month? Group awards? Thank you notes to nursing and ancillary staff for the “little” things? Do you remember birthdays? Does the group grant titles for special situations? A director of quality? Readmissions? Transitional Care? Diabetes? Recognize and reward. Sometimes promotions, a dinner, or a thank you, can go further than a monetary reward.
Once these areas, perhaps not stepwise, but more likely in concert, are achieved, you will begin to reach the top of the pyramid. It’s at this level that individuals and the group will find they want to reach beyond themselves and help make the hospital and the group better. The complaints that take up the day will be flipped into ways to improve together.
There are many steps to success. This is one simple framework that begins to shape how we can motivate each other, together, to make hospital medicine the best team in the game.
Follow the footsteps of Maslow and Messler, and you will be on the path to engagement and high performance.



Dr. Jordan Messler offers excellent words of wisdom. His hierarchy is very helpful.
Messler strives to bring professionalism, recognition, humanity and mutual respect within a system challenged by budgetary constraints & bureaucratic expectations of more from fewer pulling the heavier weight of growing case loads. It takes courage & strength to avoid burnout or compromise of professional ethics. Love your family first and be true to yourself!
Nice try Dr Messler. May I suggest that there is rarely a utopia. Utopia is an illusive destination and too often just a dream not easily described . However, it is more easily envisioned when “Engaged” is at the bottom of the Hierarchy Pyramid. Engagement is not the destination. . Engagement is the ingredient that facilitates the foundation of the pyramid. Enhance engagement and you can more easily attain growth in the pinnacle of Maslow/Messler hierarchy of needs.
Great Post!