I recently read the following written by Daniel Ofri, MD in the NYT:
The stereotype of specialists handling the more complex and intellectually challenging cases makes many generalists fume. Generalists observe that specialists get the “simplicity” of handling very narrow slivers of medicine. It’s much easier to be an expert when you only have a handful of diseases to worry about. And any issue that a specialist doesn’t want to deal with can be permissibly kicked back to the generalist.
The generalist, however, gets no dispensation. Every issue that the patient raises must be addressed. Every symptom from any organ has to be acknowledged. Plus, every medication prescribed by every specialist must be accounted for. Every competing interest between the many medical cooks in today’s fragmented health care environment must be integrated.
It brought to mind something else I saw of late–Modern Healthcare’s physician compensation survey. The publication obtained data from eleven firms reaching a combined 6,550 healthcare organizations and nearly 346,000 physicians.
What you will note below are the five lowest paying medical specialties. Happy times have not visited primary care. Notice the white expanse between the cluster at the top and the stragglers at the bottom:
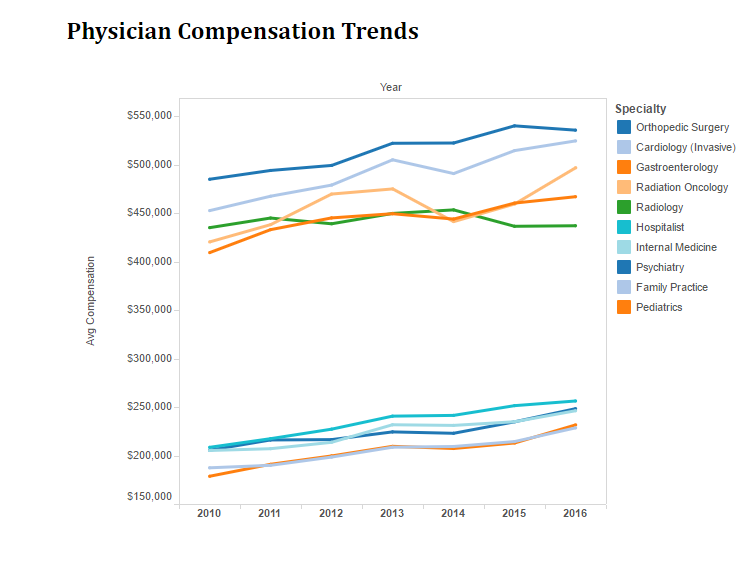 You also might be surprised to see hospitalists in the same cohort as peds, psych, FP, and IM. I was under the impression hospitalists garnered a higher premium than the rest and in particular, internists on the ambulatory side–the actual apples to apple comparator. When I looked at 2014 data, median compensation and collection per RVU were about equal. Mileage varies by region and employer, but for the most part, the numbers fell within 5-10% of each other.
You also might be surprised to see hospitalists in the same cohort as peds, psych, FP, and IM. I was under the impression hospitalists garnered a higher premium than the rest and in particular, internists on the ambulatory side–the actual apples to apple comparator. When I looked at 2014 data, median compensation and collection per RVU were about equal. Mileage varies by region and employer, but for the most part, the numbers fell within 5-10% of each other.
But why have we seen this migration away from IM primary care towards inpatient medicine if there is only a small salary dividend? Furthermore, if ambulatory care rejuvenates itself and the dollars ramp up and the quality of life on the outpatient side of practice rights itself, and I am only speculating, will hospitalists and the 7-on/7-off plus night and weekend drudgery drive internists back to ambulatory care? If the laws of supply and demand hold, will doctors at some point say, “275K plus in the office or 265K on the wards…and what am I doing wrong here?”
Since I left training, I believed every principal in healthcare laid waste to primary care due to the “irrelevance” of the field–born from revenue and clinical ruin. However, I am beginning to rethink how the next decade will appear. CMS and the ACP like to trumpet some of the crumbs payers are tossing out to primary care practitioners. Not nearly enough, but in viewing the logistical and economic forces at the macro level–too hard to ignore and at times resembling an oncoming freight train, the system will recast itself. Just something I saw of late (but by no means conclusive):
Depending on the number of patients participating, providers can earn an additional $100,000 to $250,000 per year under the model, according to Lynn Barr, chief transformation officer at Caravan Health, a healthcare consulting firm.
I am also noting recruiter ads with big perks along with what seems like attempts to not just hire but to retain ambulatory docs for the long haul. Given the dreadful state of the specialty, I know tiny sprouts of hope a transformation doth not make, but it’s a ripening trend. It could be noise, but I don’t think so. I am also observing a lot of attention being paid to burnout (and programs initiated to prevent it)–the scourge of our profession.
Also, the choice is not only dollars (although it likely is), and job satisfaction encompasses many things: autonomy of decision-making, professional fulfillment, love of practice setting, and quality of life. But it makes me think why hospital medicine grew in the first place.
The counterfactual, and it’s a biggie, would have been a kind and functional ambulatory world no one wished to abandon. Would people have packed up shop then and left the field to move into the hospital? Moreover, I would even rephrase the question and ask whether hospital medicine pulled providers away or rather, did ambulatory care push them? Divisions don’t develop in adaptable, happy places when the participants like their work. The distinction has implications for the future.
“This has all been an economic move,” she says. “People sort of forget that, I think. It [hospital medicine] was discovered by some of the HMOs on the West Coast, and it was really not the HMOs, it was the medical groups that were taking risks—economic risks for their group of patients—that figured out if they sent … primary-care people to the hospital and they assigned them on a rotation of a week at a time, that they can bring down the LOS in the hospital.
How do we explain the germination of our field:
Broken markets and the regulatory machine. Worker demand under normal circumstances increases wages–which did not occur in primary care. But hospitals, profit centers, did find a way to pay hospitalists–from a more lucrative pot of inpatient dollars. The distortions shifted docs from a deprived to a more profitable sector. It did not happen because the higher ups allocated providers to maximize outcomes and do what was best for our system. Keep in mind also; most hospitals will soon become cost centers. The go-go days are fading.
The hospitalist model evolved because of changes in hospital demography and the need for greater oversight. Again, if ambulatory care was better reimbursed and functional, innovations beyond the “creation” of hospital-based docs might have, and likely answered the call. I could have envisioned tech, quality, safety, and transitions being handled by other innovative divisions formed anew.
Advocacy: Hospital medicine was quick to organize and strike while the iron was hot. Frustrated and ambitious docs (myself included) picked up the ball. Our peers in cardiology, GI, and pulmonary saw no such need. They already had their boards, specialty designation, codes and cash flow written into stone. Maybe the movement was so great and convincing it demanded immediate advocacy, and everyone fell in behind. Or maybe we just got lucky. Nature abhors a vacuum. It happens sometimes.
Hospital as laboratory: I don’t believe the “hospital as the truly broken site” versus the outpatient setting was the impetus for the inpatient manpower influx. For every defect and adverse outcome, the ambulatory setting had a parallel case. The excess comorbidity and mortality there just manifested in more stealthy ways.
Disavow yourself of the notion hospital medicine will disappear. However, as quickly as the forces arose that turned on the growth spigot they could also diminish and bring to bear a slowdown and a slamming of the brakes. When that occurs any exodus of personnel you might see will have less to do with a fade of hospital medicine; rather, it may have more to do with a return to the field that sent them packing initially. Folks didn’t leave offices because acute care institutions built a better mousetrap. They left because no one fed the cat in the structure they abandoned.
“The fact that primary care physician again took another double-digit increase—it’s over $200,000 for the first time, it’s $225,000—I think it’s notable,” said Singleton. “The way our system is designed, it rewards procedures and punishes diagnoses. For a primary care physician to make such huge jumps year after year in compensation really shows you where we’re at in that market–it’s a well-deserved bump for them.”



[…] Are hospitalists paid like specialists or primary care docs? Any why? Brad Flansbaum of The Hospital Leader investigates. […]