While driving into work earlier this week, I heard a wonderful interview with Jim Dierke, principal of Visitation Valley Middle School here in San Francisco. VV is one of the poorest neighborhoods in the city, and this gentleman – who recently won a national middle school “principal of the year” award – has managed to increase attendance rates above 90%, get the kids engaged in their studies, and enlist the help of community service providers and donors. He’s a rock star, and the interview was inspiring.
But he had one concern: the 2001 “No Child Left Behind” law. While noting that increasing the focus on math and reading was probably healthy, he lamented that
these standards are very good, but they are in a very narrow scope. In order to meet [them], we’ve had to really narrow the focus of education. And so music, art, computer literacy, librarians, social workers… we’ve had to eliminate and pare down in order to put the emphasis on No Child Left Behind. At the same time, this has resulted in kids learning a little more in English and in math, which we want them to do, naturally, but it has narrowed their focus on becoming a well rounded, well educated person..
Like any good leader, he’s been hustling to raise money to bring some of this “soft” content back into his school, but he has been only partly successful.
His experience is not unique. The chart below shows the enrollment in San Diego School District music classes in 1999 and 2003 (before and after NCLB).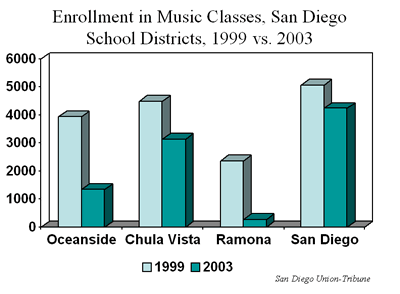
This, of course, is one of the big unforeseen consequences of quality measurement, at least in its present incarnation in healthcare. Even if the measures are all well grounded in science (and many of them are not, a point I’ll return to in the next few weeks), they inevitably cause people and organizations to play for the test.
At my hospitalist conference last week, this issue really struck home during a “Clinical Problem Solving Exercise” session. I presented an unknown case to Gurpreet (“Goop”) Dhaliwal, an assistant professor at our San Francisco VA Hospital. Goop is an astoundingly good diagnostician; he’s like Gregory House without the attitude. The case was hellishly complicated: culture-negative endocarditis, emboli everywhere – it had more twists and turns than Lombard Street; more red herrings than my grandma’s breakfast table. As usual, Goop was all over it, combining astounding deductive abilities (and a preternatural ability to think on his feet in front of 600 people; I would aspirate if put in a similar situation) with a fund of knowledge that would do Google proud.
Believe me, if you came into the hospital really sick and you had a choice, you’d want Goop, and not me, to be your doctor. But I might well do better on the publicly reported quality measures. After all, they aren’t rocket science: performing well on them can be accomplished with a good checklist or, better yet, a computer system that hardwires them in place (though this isn’t as easy as it sounds).
I’m afraid that Goop’s diagnostic acumen might well be healthcare’s music class: extraordinarily impressive, really quite beautiful in a way, but way off the measurement radar screen. If our students get the message that Goop’s kind of clinical intelligence and diagnostic ability are unimportant (after all, they don’t seem to be part of what we’re calling “quality”), I think you can guess what will happen over time. Clinical “artists and musicians” will become extinct.
That, my friends, will be a big loss.


Leave A Comment