by Leslie Flores, MHA, SFHM
Does paid time off (PTO) make sense for physicians like hospitalists and ED docs who are largely shift workers? I guess it depends on your perspective, though I have some definite opinions of my own. But before sharing my thoughts on the value of PTO for hospitalists, it might be instructive to understand a bit about the current state of PTO in hospital medicine groups.
 It’s hard to know what to make of the information that’s currently available about PTO for hospitalists. Only about 31% of hospital medicine groups serving adult patients provide some paid time off, according to SHM’s 2014 State of Hospital Medicine Survey, though the prevalence of PTO is much higher in academic groups (55%) than non-academic groups (27%). And academic groups provide a median of 208 hours of PTO annually while non-academic groups provide a median of 120 hours annually. But oddly enough, the median number of shifts worked per year is exactly the same for both academic and non-academic hospitalists at 182.
It’s hard to know what to make of the information that’s currently available about PTO for hospitalists. Only about 31% of hospital medicine groups serving adult patients provide some paid time off, according to SHM’s 2014 State of Hospital Medicine Survey, though the prevalence of PTO is much higher in academic groups (55%) than non-academic groups (27%). And academic groups provide a median of 208 hours of PTO annually while non-academic groups provide a median of 120 hours annually. But oddly enough, the median number of shifts worked per year is exactly the same for both academic and non-academic hospitalists at 182.
The SHM survey also tells us that hospitalists employed by hospitals or integrated delivery systems are much more likely (47%) to receive a PTO benefit than hospitalists employed by private hospitalist groups (5%) or management companies (3%). A surprising 78% of pediatric hospitalist groups offer a PTO benefit. 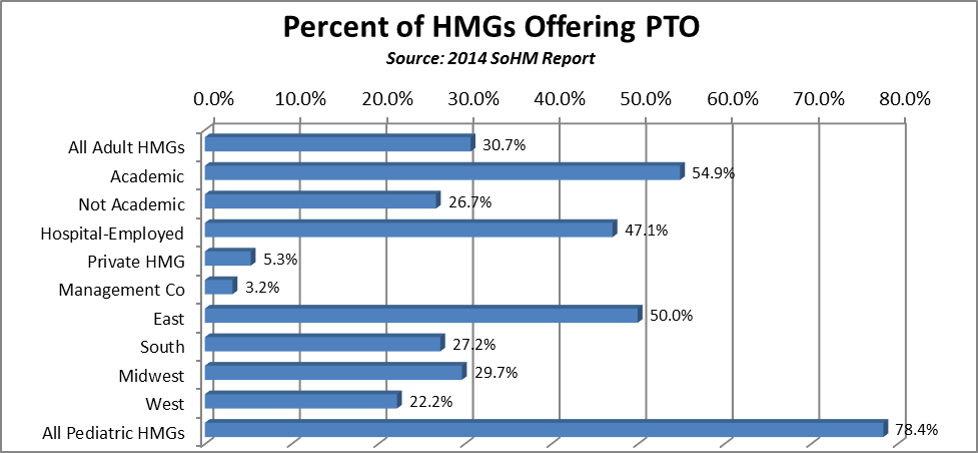 And if you’re a hospitalist in the northeastern quadrant of the U.S. you’re more likely to have access to PTO than if you live in other parts of the country. And here’s something else interesting: the larger your group is the more likely you are to have PTO, and the more hours of PTO you are likely to accrue annually. But none of these factors appear to significantly impact the actual number of shifts hospitalists actually end up working annually; the median is right around 182 shifts, pretty much across the board.
And if you’re a hospitalist in the northeastern quadrant of the U.S. you’re more likely to have access to PTO than if you live in other parts of the country. And here’s something else interesting: the larger your group is the more likely you are to have PTO, and the more hours of PTO you are likely to accrue annually. But none of these factors appear to significantly impact the actual number of shifts hospitalists actually end up working annually; the median is right around 182 shifts, pretty much across the board.
Most – but not all – of the work my consulting partner John Nelson and I do is with adult medicine hospitalists employed by hospitals or integrated delivery systems, and our experience is pretty consistent with these survey results. A meaningful minority of the groups we’ve worked with offer some paid time off benefit, and I think the proportion of groups doing so is increasing slowly as the specialty of hospital medicine matures. We do find that most groups offering PTO have a base schedule of something less than 182 annual shifts. Most often it’s two seven-day weeks of PTO annually, with an expectation to work a base schedule of 168 shifts a year. But what we tend to find is that these groups often don’t have the extra manpower needed to cover the paid time off, so the hospitalists tend to cover each other’s PTO by working extra shifts. So the PTO “benefit” often doesn’t really result in the intended benefit of longer blocks of time off to rest and recuperate but instead result in working just as many shifts as those without PTO – but earning some extra money.
So back to my original question: does PTO make sense for hospitalists? Based on my experience, there does seem to be real psychic value for some folks in knowing they have access to something that’s considered part of the standard benefits package for most U.S. employees. This may be especially true for hospitalists who work in a group that employs a strict seven-on/seven-off schedule in which it’s otherwise hard to get more than seven consecutive days off. And for people who value the opportunity to earn more money by working extra shifts to cover their colleagues’ PTO more than they value additional time off for themselves, PTO is a decidedly good deal.
For most hospitalists, though, I think a formal PTO benefit shouldn’t be necessary. What should really matter to hospitalists is that they are compensated fairly for the work they do, and that they have generous amounts of time off – in increments that are useful to them – to make up for the long, stressful work days and the high proportion of weekend and night work that most of them do. If these things are in place, why would you want your employer to hold back part of your guaranteed pay just so it can be paid to you for some arbitrary portion (but not all) of the days you are not scheduled to work?
If you ask your emergency medicine colleagues whether they get PTO, they’ll probably look at you funny and say, “I don’t know; all I know is that I have to work 15 shifts a month.” ED physicians, unlike hospitalists, don’t need to worry about continuity. So they have much more flexibility in how they schedule their 15 monthly shifts, and can easily schedule longer blocks of time off when they need to. I think the ‘need’ for PTO in hospital medicine has come about because so many of us have tied ourselves to a rigid seven-on/seven off schedule. Access to PTO is too often seen as the only valid way to get more than seven days off in a row. No one wants to have to work 21 days in a row just so they can have two consecutive weeks off like the average American. I’m sympathetic.
Will the presence of PTO in hospitalist benefits packages continue to increase? Despite my contrarian opinion, I’m guessing it will. The specialty is maturing and – unthinkable just a few years ago – large numbers of hospitalists are starting to age into their 50s and even 60s. Older hospitalists are finding it especially challenging to continue working seven-on/seven-off schedules without a meaningful break occasionally. In settings where no PTO is available we’re starting to see some experienced hospitalists move to part time clinical roles and pursue other administrative and medical leadership options in their organizations in order to get some relief from the systole-diastole lifestyle.
Perhaps increased access to PTO will provide a mechanism to help hospitalists continue in the specialty as they age. Personally, I think an even more powerful aging-in-place incentive will be a willingness to consider more flexible scheduling options that allow for a varied work schedule and generous amounts of time off in meaningful increments. It will be interesting to see what trends the next SHM survey in 2016 shows.
I know this is a potentially controversial topic, and others will have different opinions. Please feel free to submit a comment below, and perhaps we can get a robust discussion going about the pros and cons of PTO for hospitalists.
 Leslie Flores, MHA, SFHM, is a founding partner at Nelson Flores Hospital Medicine Consultants (www.nelsonflores.com), a consulting practice that has specialized in helping clients enhance the effectiveness and value of hospital medicine programs as well as those in other hospital-focused practice specialties since 2004. Ms. Flores began her career as a hospital executive, after receiving a BS degree in biological sciences at the University of California at Irvine and a Master’s in healthcare administration from the University of Minnesota. In addition to her leadership experience in hospital operations, business development, managed care and physician relations, she has provided consulting, training and leadership coaching services for hospitals, physician groups, and other healthcare organizations. Ms. Flores is an active speaker and writer on hospitalist practice management topics, and serves on SHM’s Practice Analysis and Annual Meeting committees. She serves as an informal advisor to SHM on practice management-related issues and helps to coordinate SHM’s bi-annual State of Hospital Medicine survey.
Leslie Flores, MHA, SFHM, is a founding partner at Nelson Flores Hospital Medicine Consultants (www.nelsonflores.com), a consulting practice that has specialized in helping clients enhance the effectiveness and value of hospital medicine programs as well as those in other hospital-focused practice specialties since 2004. Ms. Flores began her career as a hospital executive, after receiving a BS degree in biological sciences at the University of California at Irvine and a Master’s in healthcare administration from the University of Minnesota. In addition to her leadership experience in hospital operations, business development, managed care and physician relations, she has provided consulting, training and leadership coaching services for hospitals, physician groups, and other healthcare organizations. Ms. Flores is an active speaker and writer on hospitalist practice management topics, and serves on SHM’s Practice Analysis and Annual Meeting committees. She serves as an informal advisor to SHM on practice management-related issues and helps to coordinate SHM’s bi-annual State of Hospital Medicine survey.



In my opinion PTO is a recruiting gimmick. Nothing more.
I totally agree with the statement that Hospitalist do need paid time off , even if it’s only a werek or two, as it will give them a flexibility to take 2 weeks off without having to pay back and work continuous 3 week shifts if they are required to payback.
A continuous 3 week shift for anyone will be
backbreaking and annoying, and the fatigue in your continuous 3rd week will definitely affect patient care.
Asif Jan
Our Hospitalist group works 15 days per 28 days cycle to allow for 13 days to take off as vacation when desired. Recently our HR department decided to change from giving out sick time days to giving 5 extra days of PTO but the administrators are having a hard time justifying giving us an additional 5 days of vacation so they are considering just removing our sick leave without giving the extra 5 days off. Has anyone else changed from sick leave to PTO?
Great topic!
Bryan, can you tell me more about your schedule model?
I have different groups of which all have various forms of time off. Key things to keep I keep in mind when analysing schedule models..
1. Is it meaningful? Does the hospitalist have to work longer shifts to get the time?
2. How do you cover time off in a way that does not burn out others in the group or blow the budget?
3. Total average shifts and hours per month/year
4. How is continuity of care and patient care potentially compromised.
I believe we will see schedules evolve as HM matures. It is important to continually evaluate as the group dynamics change. Striking balance is difficult but thinking out of the box can often result in win/win models.
Thanks Leslie for the topic!!
I think that this is a very controversial issue. With a 7on/7off schedule one would expect hospitalists to have enough time off, but the issue to consider would be the duration. The flexibility to take longer periods of off/vacation time is a benefit of PTO. This would otherwise not be possible in groups due to demands of scheduling. I this is a faction in increasing longevity and reducing burnout in hospitalists.
Thanks.
Rupesh.
Leslie,
This is a very important topic and one that I encounter on a weekly basis. Let me start by stating my bias: PTO should not be part of hospitalist agreements.
Essentially, we need to more closely examine the reason for PTO and recognize that our current strict 7on/7off model (employed by most HM programs) is not sustainable. Even though we have made good strides over the past few years, we still have the all important issue of creating a “destination career” for many of our providers.
The more important topic is the one raised by your blog piece – should we better define FT hospitalist? Should the definition be closer to 168 shifts rather than the current 182? Would this decrease the chances of burnout and therefore prolong ones clinical career? I suspect so. The other thought surround the duration of each shift. Should we consider shifts that are 8-10 hours instead of 12.
I fall squarely on the side of shorter shifts, redefining the FTE in HM and much like most ED programs, eliminate PTO.
O’Neil.
Thanks to everyone who has commented, both here and on HMX! I really appreciate the diversity of opinions expressed, which demonstrate the strong feelings people have around this topic.
O’Neil, I wanted to respond specifically to your comment about whether the common definition of full time should move from the current 182 toward something like 168, vs. shorter shift lengths. I think we see this similarly.
What if hospitalists, instead of working fewer days annually, actually worked MORE days annually than they do now? I’m not suggesting that hospitalists would see more patients or do more work in total – just that the work they’re currently doing might be titrated out differently and in a way that is arguably more sustainable.
For example, instead of working 182 12-hour shifts (2,184 hours annually) and seeing 15 patients a day, a hospitalist group agreed everyone will work 210 10-hour shifts (2,100 hours annually). Roughly the same number of hours, and the same volume of patients. So the daily average patient volume would go down from 15 to about 13.
The hospitalists would have fewer days off annually, but if combined with a flexible schedule that accommodates longer increments of time off when needed, many hospitalists might find working a little less hard each day they work more appealing.
The decision of whether to offer PTO under this or any other staffing model really just becomes one about how the available pay for each hospitalist is doled out – the really important factors are how much work is expected, whether it’s structured in a way that’s sustainable, and whether the compensation is fair for the work being done.
— Leslie