Think of the drunk looking for his lost car keys under the only light post in a parking lot. As unlikely as he might find the keys, he does use logic in his approach despite his low odds of success.
We use readmits for the same reason. We have mediocre tools to assess outcomes, but nothing better exists. We use readmissions because we do not have much else to employ.
If one could equate a hospital stay to a restaurant experience, readmits as part of our composite grade would rank somewhere between arranging the table china and the linen choice. And like the décor and individual courses do not approximate the whole of the dining encounter, nor does a return trip fully capture what transpires under the hospital roof during an inpatient stay. Too many variables coexist—indeterminate to provider control—and we cannot illuminate how physician, hospital, ancillary staff, patient, and community interact and contribute to the outcome.
Yes, as a country, we have improved—readmits have dropped 1-2% in absolute terms the last few years. However, we do not know precisely why, nor have confidence in what interventions we have implemented to make the strides. We also cannot determine whether the hospital can take full responsibility for the downtick.
I doubt the drop has contributed much to the recent decrease in per capita health spending, much to the chagrin of those touting the decline as the raison d’etre for our systems’ recent efficiency shift. Preventable readmits do not factor much into our large health care price tag. It is also hard to claim any positive externalities impacting other aspects of care from whatever practice changes we have adopted, given we cannot reliably identify them. They exist, but to many physicians, including me, no one has told us the blind folds came off.
Without getting too scientific, underneath I list core bits of what we know on readmissions and their prevention as of today:
1. Not one intervention has magic bullet status. Most studies indicate success involves the interplay of many items, often involving people outside the hospital in the community.
2. Medication reconciliation, patient education, family involvement, and follow-up appointments matter—but not to everyone and we do not know if we should apply them to each patient or use them selectively.
3. The thirty-day window of measurement for penalties places us in a no-win position. Based on our actions at discharge, we probably affect days 1-14 only.
4. Adjusting outcomes for hospitals caring for patients of lower socioeconomic status may (or may not) make a difference. The data lacks clarity at present.
5. Preventable readmissions remain a mystery as a percent of total readmissions. Based on my read, the low could be 5% and the high could be as great as 20%.
6. Most readmissions arise secondary to diagnoses unrelated to the initial one.
7. Favorable readmission rates may (or may not) correlate with hospitals possessing superior patient experience or mortality scores.
8. Regulators do not seem to be asking who should be accountable for deficiencies in the community safety net leading to return trips; rather, the hospital message I hear is “tag, your it.”
9. Administrative claims data, as used by the readmission measure, correlate poorly with clinical data derived directly from medical records.
The consequence of this uncertainty? We cannot embrace and own the outcomes. We can’t “feel” the data.
I admit approximately 600 folks per year. If I include all payers, figure a readmit rate of 15%. Over twelve months, 90 of my patients return. The difference between a top performer—a colleague of mine at 13% per year—and myself, would be 12 patients.
For most of us, with readmit incentives incorporated into our pay, we will forgo a good chunk of change owing to the above. Next year when we reexamine the data, my colleague regresses to the mean (again, on accord of many non-correlated inputs). The bonus will reverse; we can investigate why her twelve patients “returned” and she can then relocate to the remediation class. I will have to relinquish my chair.
The readmit metric has a long way to go—both on the knowledge discovery front and how we as practitioners should seek wisdom in a very crude measurement. I am still amazed at how many non-clinicians find meaning in a measure so few clinicians view as high impact. You just need to speak with us.
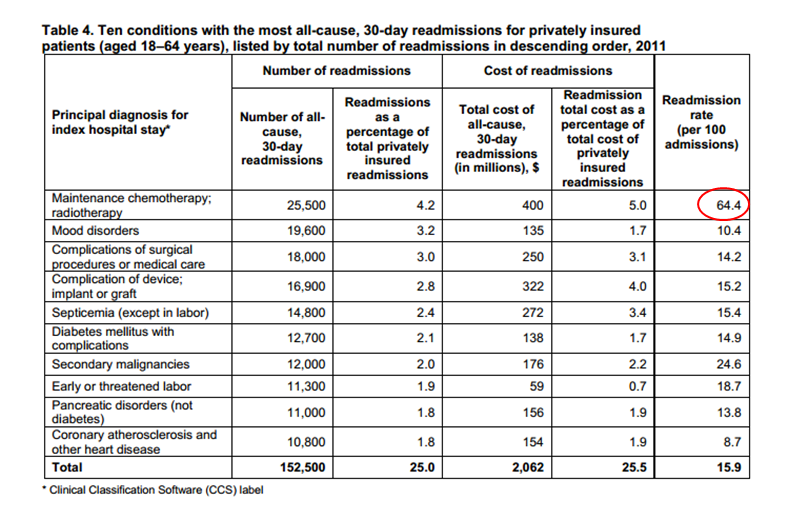
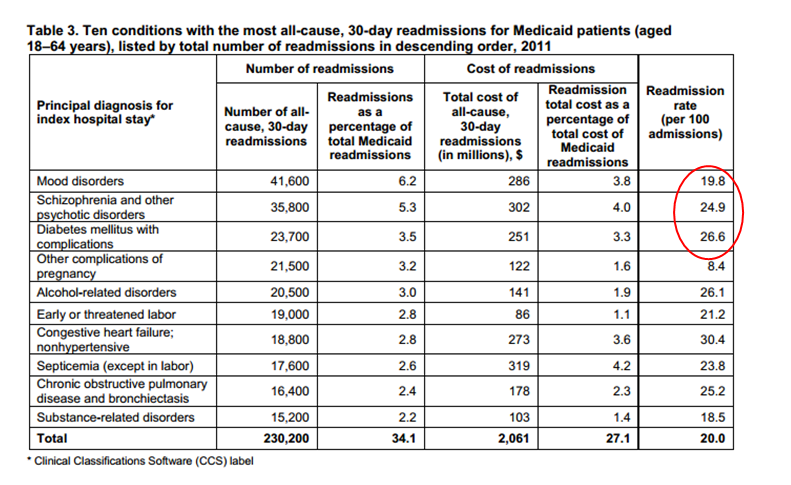
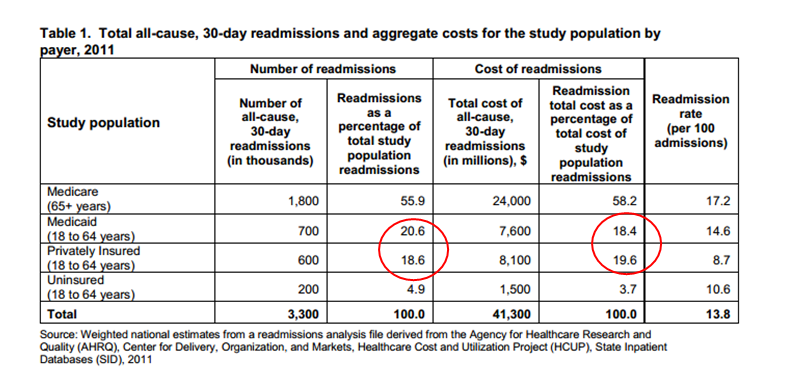
I want to conclude with some HCUP data below (red circles mine) and questions.
If I asked you the top readmit DRGs for commercial and Medicaid plans, would you know? Do they too have relevancy along with the Medicare diagnoses we focus on closely—sometime to the detriment of everything else? Do they likewise have merit and add costs to the system? And finally, do the interventions we utilize for MI, CHF, and PNA patients have different effects on Medicaid and commercial folks, and if so, why?
Just something to think about.
UPDATE: After writing the above post, I came across a terrific JHM early release that conveys a similar message. An outstanding piece and the commentary deserves a read.


Very insightful article. I suspect over time, with the addition of continued analysis of the matrix, here will be a clearer understanding of the readmit issues. Just as with insurance, with enough data and a sufficient census, there should be better predictability of readmissions.
Extrapolating your thoughts to a related topic: http://runningahospital.blogspot.com/2014/07/admissions-about-readmissions.html
[…] effects are brought to our attention by Bradley Flansbaum at The Hospital Leader. In his post, “PNA, CHF, MI. RInse. Repeat,” he notes, “Reductions in readmissions get outsized attention for reducing health system costs […]