By now, you’ve probably heard the news: providing a price transparency tool to patients does not seem to lower healthcare prices. In fact, according to this very large JAMA study, patients who were offered access to a price transparency tool seemed to spend slightly MORE compared to those patients without access. So, I guess put that whole price transparency idea to bed.
Well, perhaps not so fast.
As Dr. Kevin Volpp thoughtfully points out in his accompanying editorial, this study shows that price transparency tools will not be a “panacea” by themselves (who actually thought they were going to be in the first place?), but that there are many important considerations for interpreting the results of this study.
I think by far the most important caveat is that the tool only included cost information, without any real context. Think about this for a second. When looking at a long wine list at a fancy restaurant, how often do you pick the cheapest bottle? Those of us that are not serious wine connoisseurs generally make judgments of relative quality based on price. The more expensive the bottle, presumably the better it is. Now think about if you will only have to pay the first $50 for that bottle of wine, no matter which one you pick, and somebody else will pick up the rest of the tab. In the study, most patients who actually used the tool (which was a mere 10% of patients that had access to use the tool) were searching for services that are higher than the highest deductible, so any differences in cost would not have directly mattered to them anyways. Yeah, price transparency is no panacea. No kidding.
the cheapest bottle? Those of us that are not serious wine connoisseurs generally make judgments of relative quality based on price. The more expensive the bottle, presumably the better it is. Now think about if you will only have to pay the first $50 for that bottle of wine, no matter which one you pick, and somebody else will pick up the rest of the tab. In the study, most patients who actually used the tool (which was a mere 10% of patients that had access to use the tool) were searching for services that are higher than the highest deductible, so any differences in cost would not have directly mattered to them anyways. Yeah, price transparency is no panacea. No kidding.
Now, with the wine list, I could turn to the sommelier and get expert information. They can give me a sense of value. The sommelier is there, ready and happy to help, and I don’t have to make an appointment weeks from now nor navigate phone trees or gatekeepers to get to them.
We must be able to immediately imagine what a better tool for patients would look like. Perhaps one that is useful enough that more than 10% of patients would even bother logging in.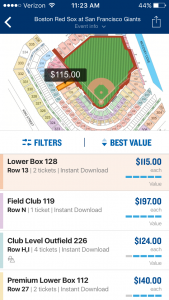
The popular secondary market ticket seller, StubHub recently introduced a “best value” sort option, which “empowers fans to quickly identify great deals, experience more clarity during the ticket discovery process, and make more informed purchasing decisions.” That’s right, you will now be better informed about the value of your concert seats than where to get a colonoscopy. StubHub created a “sophisticated algorithm” behind the new best value filter that leverages its own historical data, as well as price, location, and availability.
The widely discussed JAMA study is immensely useful in showing us all what not to do. You cannot simply introduce a clunky tool that nearly nobody uses, without context, and expect results. We can do better. True, defining value in healthcare is interminably more complicated and entails higher stakes than seats at the next Beyoncé concert, but shouldn’t we, as a $3 trillion per year industry, be at least as good as StubHub? How can we accept anything less?



Leave A Comment