We all walk into the supermarket and see an abundance of goods. Every item has a place under alluring lighting and come-hither ads. The displays move you and your wagon, despite your beliefs, through the aisles in a deliberate way. The Walmart Supercenter manager wishes to steer your senses so as to induce the transfer of maximal amounts of merchandise from the shelf to your basket (and money out of your wallet). You don’t think Whole Foods places huge reams of flowers at the entrance to their stores just to remind you of Mother’s Day, do you?
There is a reason for everything. Menu layouts, web page designs, product placement (I love this), commercial advertising–it’s so subtle that the subtly washes over us. We think we have codebook, but really, most of the time we do not have a clue.
I like paying attention to this stuff, though. Since my college days, I have always walked into stores, car dealerships, or watched movie trailers to interpret the marketer’s intent. How the creators of promotional material wish to prompt us or make us behave makes for a challenging pursuit.
But like the greatest deceptions, you never really know when you have been snookered; when the desired message has reached your cortex and had an effect. I would not describe the effect as evil–we are not talking mind control a la Manchurian Candidate, but one if recognized leaves you feeling a tad exploited. Not a biggie most of the time and life moves on.
These prods can be corrective in a positive way.
When your CFO, medical director, chief, or direct report institutes a pay for performance scheme, could they approach the exercise in a similar manner using corresponding methods. Do they see providers as less than optimal in how they make their practice decisions? And if so, could they prompt them down an alternative care path; one more ideal for patients than the one they ordinarily veer down.
What should go into their formula and how can they structure the payout to motivate us in the most efficient manner then? For example, should we get our bonus in advance, say in January, or at the end of the year? Should we get any earnings in a lump or divided sum? How much of our take home should be at risk and who should be the target–just the individual or the group? The bean counters have much to consider.
If you have not gotten it by now, I am referring to behavioral economics.
Doctors often fail to act in an expected way. So if you want to steer them in the right direction, you have to flip the right switches and get them to respond to cues.
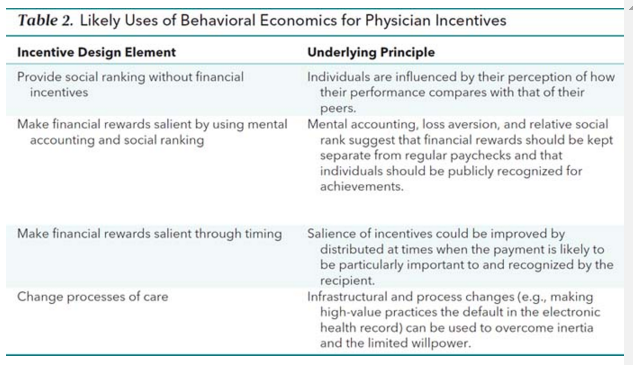
Hence, I wish to recommend a review just released from the Annals of Internal Medicine, entitled: Using Behavioral Economics to Design Physician Incentives That Deliver High-Value Care. In it, you will find a basic primer on how to shape better performance using behavioral techniques.
The figure below summarizes a portion of the article, but for me, some of the takeaways include (my comments in parenthesis):
- Pay bonuses frequently and up front. Clawback shortfalls on the back end.
- Make goals close enough to achieve, but not too close (seems obvious, but most of the goals I have encountered lean more towards aspiration x two, e.g., HCAHPS scores and readmit rates).
- Issue group report cards (with caveats as data should be clean with outliers removed).
- Use a mix of group and individual targets with emphasis on the latter.
- Keep enough money at risk (probably 10-20%, but no more).
Read the article for the full treatment–it is a fine summary of behavioral basics. Moreover, if you especially like the subject, pick up any of these three standards. If you want the books with the Jedi mind tricks, I cannot help you there. Try Amazon.



Hi Brad,
Thank you for a great analysis on a thought-provoking article. As health care organizations focus on high value care, I think it is important to use a combination of two or more incentive elements to engage more providers and achieve better results. At the same time care as the authors rightly state, care should be taken to maintain a balance between performance metrics and availability of options.
Rupesh.